What causes intrathoracic pressure
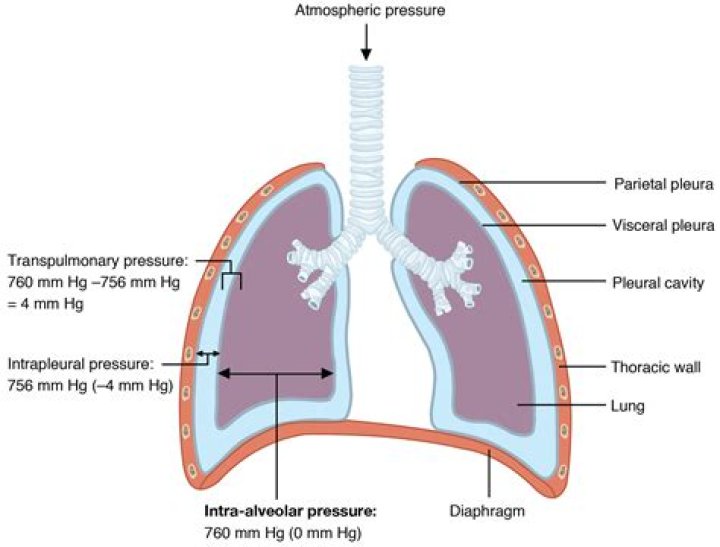
The changes in intrathoracic pressure during the respiratory cycle are mainly caused by the changes in the intrapleural pressure that is transmitted to all intrathoracic pressure values (Boerrigter et al., 2014).
What increases intrathoracic pressure?
Third, positive-pressure ventilation increases intrathoracic pressure. Since diaphragmatic descent increases intra-abdominal pressure, the decrease in the pressure gradient for venous return is less than would otherwise occur if the only change were an increase in right atrial pressure.
Does exercise increase intrathoracic pressure?
Exercise influences these cardiopulmonary interactions by augmenting the fluctuations in intrathoracic pressure (ITP) and altering the depth and frequency of breathing while at the same time increasing the demand for cardiac output (Olafsson et al.
What causes negative intrathoracic pressure?
Large negative intrathoracic pressures are generated during episodes of obstructive apnea. In central sleep apnea, relatively large negative pressure deflections occur during hyperpnea, particularly in the face of less compliant (stiff) lungs (due to heart failure).How does exhalation contribute to increasing the pressure in the venous system?
When cardiac output increases, blood is rapidly pumped out of veins, which reduces venous pressure (as it does not get a chance to rise). When cardiac output decreases, blood backs up into the venous system. Therefore, the blood volume increases which raises venous pressure.
Why is it important that the intrathoracic pressure be kept lower than atmospheric pressure?
Emphysema is a lung problem that casues a decrease in tidal volume. … Too much air in the lungs, this air is trapped in the lungs. Why is it important that intrathoracic pressure be kept lower than atmospheric pressure? Need a pressure gradient for air to flow in and out of the lungs.
What stimulates J receptors?
The type J receptors are stimulated during pulmonary congestion produced by occluding the aorta or left a-v junction which causes the left atrial pressure to rise with consequent rise in pulmonary artery pressure.
What's the cause of a collapsed lung?
Collapsed lung can be caused by an injury to the lung. Injuries can include a gunshot or knife wound to the chest, rib fracture, or certain medical procedures. In some cases, a collapsed lung is caused by air blisters (blebs) that break open, sending air into the space around the lung.Is intrathoracic pressure the same as Intrapleural pressure?
Intrapleural pressure is different from intrathoracic pressure. The thoracic cavity is the space that includes the pleura, lungs, and heart, while the pleural space is only the space between the Parietal pleura and visceral pleura surrounding lungs. … This is due to the recoil of the chest and lungs away from each other.
Which pressure actually keeps the lungs from collapsing?intrapulmonary pressure is what keeps the lungs from collapsing (atalectasis) due to their natural elasticity. causes lung collapse.
Article first time published onWhich of these occurs during exhalation?
When the lungs exhale, the diaphragm relaxes, and the volume of the thoracic cavity decreases, while the pressure within it increases. As a result, the lungs contract and air is forced out.
What causes negative pressure in pleural cavity?
This negative pressure is thought to be generated by the lymphatic drainage of fluid from the pleural space (Negrini & Fabbro, 1999), which occurs because of the gentle peristaltic suction of lymphatic vessel walls.
How does intrathoracic pressure affect preload?
Increased intrathoracic pressure is transmitted to cenral veins and the right atrium, decreasing right ventricular preload. Increased intrathoracic pressure is transmitted to pulmonary arteries. Transmitted alveolar pressure increases pulmonary vascular resistance.
How is a decrease in intrathoracic pressure achieved during inspiration?
Due to the adhesive force of the pleural fluid, the expansion of the thoracic cavity forces the lungs to stretch and expand as well. This increase in volume leads to a decrease in intra-alveolar pressure, creating a pressure lower than atmospheric pressure.
When does thoracic pressure increase?
Expiration. Expiration (exhalation) is the process of letting air out of the lungs during the breathing cycle. During expiration, the relaxation of the diaphragm and elastic recoil of tissue decreases the thoracic volume and increases the intraalveolar pressure. Expiration pushes air out of the lungs.
Why does arterioles decrease pressure?
As the blood vessel splits from the small arteries and into the arterioles, there is a drop in blood pressure. This drop occurs because there is an increased ratio of surface area to volume, which means that the blood is in contact with more blood vessel surface area.
How does the cardiovascular system create a region of higher pressure?
The contraction of skeletal muscles surrounding a vein compresses the blood and increases the pressure in that area. This action forces blood closer to the heart where venous pressure is lower.
Why does the pressure in the arteries and arterioles fall as the blood moves away from the heart quizlet?
Why? Blood pressure decreases, because of the effects of friction between the vessel walls and the moving blood. Blood flows through a vessel at a particular flow rate and velocity.
When J receptors are stimulated it causes?
The stimulation of the J-receptors causes a reflex increase in breathing rate, and is also thought to be involved in the sensation of dyspnea, the subjective sensation of difficulty breathing.
Why do J receptors cause rapid shallow breathing?
Because of their location, these receptors respond readily to chemicals in the pulmonary circulation, distention of the pulmonary capillary walls, and accumulation of interstitial fluid. Once stimulated, impulses travel via the vagus nerve in slow conducting fibers, leading to rapid, shallow breathing.
What do pulmonary stretch receptors do?
The pulmonary stretch receptors are nerves ending in the tracheal and bronchial smooth muscles. Their activity is enhanced by enlargement of airway cross-section, for example, when the lung volume increases, and results in an inhibition of further inspiratory activity.
What happens to the lungs if intrapulmonary pressure increases above atmospheric pressure?
Intrapleural pressure is negative relative to atmospheric and intrapulmonary during normal breathing. If intrapleural pressure becomes equal to atmospheric pressure, lung collapse will occur. … Air rushes into lungs along this pressure gradient until intrapulmonary and atmospheric pressure are equal.
Does alveolar pressure increase during inspiration?
During inhalation, the increased volume of alveoli as a result of lung expansion decreases the intra-alveolar pressure to a value below atmospheric pressure about -1 cmH2O. This slight negative pressure is enough to move 500 ml of air into the lungs in the 2 seconds required for inspiration.
How do you measure intrathoracic pressure?
Intrathoracic pressure is typically measured by monitors placed in the por- tion of the esophagus within the chest. Because of the pliability of the esophageal wall, the pressure in the esophagus generally reflects the intrathoracic pressure (Coates et al. 1989).
When the pressure in the lung is greater than atmospheric pressure?
When alveolar pressure becomes greater than atmospheric pressure, expiration occurs, and air flows out of the alveoli.
Why is negative intrathoracic pressure important to breathing What would happen if this pressure is lost?
Why is negative intrathoracic pressure important to breathing? What happens if it is lost? The pressure within the thorax is negative with respect to atmospheric pressure & creates a partial vacuum within the thorax. That partial vacuum pulls the lungs tightly out against the thoracic wall.
Can stress cause collapsed lung?
Pneumothorax patients may be included in a high-risk group of severe stress, particularly elderly patients, who can be more fragile and therefore more at risk from a pneumothorax or its related treatment. Pneumothorax is an irritating disease with a high recurrence rate that may require frequent ED visits.
Who is at risk for pneumothorax?
Risk factors In general, men are far more likely to have a pneumothorax than women are. The type of pneumothorax caused by ruptured air blisters is most likely to occur in people between 20 and 40 years old, especially if the person is very tall and underweight.
Can a collapsed lung be repaired?
Some people with a collapsed lung need extra oxygen. Lung surgery may be needed to treat collapsed lung or to prevent future episodes. The area where the leak occurred may be repaired. Sometimes, a special chemical is placed into the area of the collapsed lung.
Does smoking diminish ciliary action?
The bronchial circulation supplies blood to the lung structures (tissue). Smoking diminishes ciliary action and eventually destroys the cilia. … The paired lungs occupy all of the thoracic cavity.
When do inspiratory muscles contract?
Action: diaphragm is the main inspiratory muscle, during inspiration it contracts and moves in an inferior direction that increases the vertical diameter of the thoracic cavity and produces lung expansion, in turn, the air is drawn in.