What is a direct result of hypoventilation?
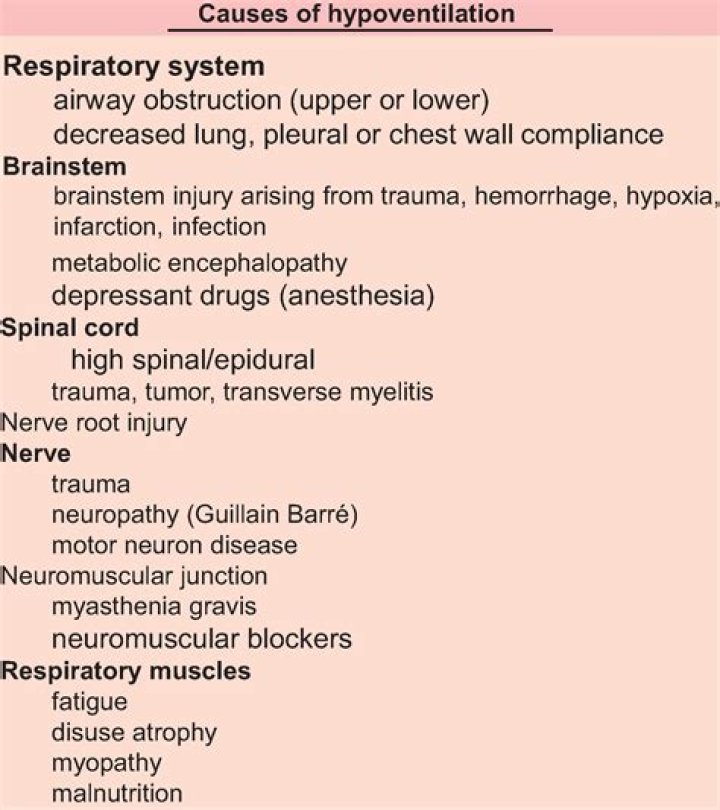
.
Considering this, how is hypoventilation treated?
Other possible treatments for hypoventilation include: oxygen therapy to support breathing. weight loss. CPAP or BiPAP machine to keep your airway open while sleeping.
Subsequently, question is, what happens when co2 increases in the body? So CO2 in the bloodstream lowers the blood pH. When CO2 levels become excessive, a condition known as acidosis occurs. Breathing rate and breathing volume increase, the blood pressure increases, the heart rate increases, and kidney bicarbonate production ( in order to buffer the effects of blood acidosis), occur.
Likewise, what causes alveolar hypoventilation?
Neuromuscular diseases that can cause alveolar hypoventilation include myasthenia gravis, amyotrophic lateral sclerosis, Guillain-Barré syndrome, and muscular dystrophy. Patients with neuromuscular disorders have rapid, shallow breathing secondary to severe muscle weakness or abnormal motor neuron function.
What is the difference between hyperventilation and hypoventilation?
Hypoventilation: The state in which a reduced amount of air enters the alveoli in the lungs, resulting in decreased levels of oxygen and increased levels of carbon dioxide in the blood. The opposite of hypoventilation is hyperventilation (overbreathing).
Related Question AnswersWhat is an early sign of hypoventilation?
During the early stages of hypoventilation with mild to moderate hypercapnia, patients usually are asymptomatic or have only minimal symptoms. Patients may be anxious and complain of dyspnea with exertion. As the degree of hypoventilation progresses, patients develop dyspnea at rest.What happens during hypoventilation?
Hypoventilation (also known as respiratory depression) occurs when ventilation is inadequate (hypo meaning "below") to perform needed gas exchange. By definition it causes an increased concentration of carbon dioxide (hypercapnia) and respiratory acidosis.What are the common causes of hypoventilation?
Some common causes of hypoventilation include:- Chronic obstructive pulmonary disease (COPD), which includes emphysema and bronchitis.
- Chest wall deformities.
- Central respiratory drive depression, which can be caused by alcohol and certain drugs, such as narcotics.
- Obesity.
- Neuromuscular disorders.
What are four signs of respiratory distress?
Symptoms of acute respiratory distress syndrome- labored and rapid breathing.
- muscle fatigue and general weakness.
- low blood pressure.
- discolored skin or nails.
- a dry, hacking cough.
- a fever.
- headaches.
- a fast pulse rate.
What are the signs and symptoms of hypoventilation?
Symptoms include:- Bluish coloration of the skin caused by lack of oxygen.
- Daytime drowsiness.
- Fatigue.
- Morning headaches.
- Swelling of the ankles.
- Waking up from sleep unrested.
- Waking up many times at night.
How is hypoventilation diagnosed?
Chronic hypercapnic respiratory failure and hypoventilation during exertion can easily be diagnosed by arterial or capillary blood gas analysis during wakefulness. However, monitoring of respiration and carbon dioxide levels during sleep are needed to establish the diagnosis of SRH.How do you fix shallow breathing?
Take a long, slow breath in through your nose, first filling your lower lungs, then your upper lungs. Hold your breath to the count of "three." Exhale slowly through pursed lips, while you relax the muscles in your face, jaw, shoulders, and stomach.What happens if hyperventilation is left untreated?
Low carbon dioxide levels lead to narrowing of the blood vessels that supply blood to the brain. This reduction in blood supply to the brain leads to symptoms like lightheadedness and tingling in the fingers. Severe hyperventilation can lead to loss of consciousness. For some people, hyperventilation is rare.What affects alveolar ventilation?
Alveoli. Minute ventilation is the tidal volume times the respiratory rate, usually, 500 mL × 12 breaths/min = 6000 mL/min. Increasing respiratory rate or tidal volume will increase minute ventilation. Dead space refers to airway volumes not participating in gas exchange.What is obesity hypoventilation syndrome?
Obesity hypoventilation syndrome (OHS), also known as Pickwickian syndrome, is a condition in which severely overweight people fail to breathe rapidly or deeply enough, resulting in low oxygen levels and high blood carbon dioxide (CO2) levels.Does hyperventilation increase co2?
Hyperventilation, sustained abnormal increase in breathing. During hyperventilation the rate of removal of carbon dioxide from the blood is increased. As the partial pressure of carbon dioxide in the blood decreases, respiratory alkalosis, characterized by decreased acidity or increased alkalinity of the blood, ensues.What is Ondine's curse?
Ondine's curse—more appropriately known as congenital central hypoventilation syndrome or CCHS—is a rare, severe form of sleep apnea in which an individual completely stops breathing when falling asleep. It is usually congenital, meaning that it is present from birth.How is co2 retention treated?
Options include:- Ventilation. Share on Pinterest Non-invasive ventilation, such as a CPAP mask, may help to treat hypercapnia.
- Medication. Certain medications can assist breathing, such as:
- Oxygen therapy. People who undergo oxygen therapy regularly use a device to deliver oxygen to the lungs.
- Lifestyle changes.
- Surgery.